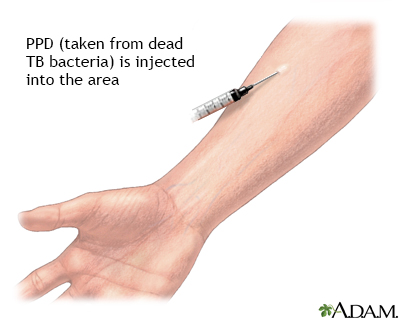
To dilute the concentration of contaminants in an isolation room, the room must: In a health care setting, infectious individuals should be placed in private (isolation) rooms. However, exposure to people with undiagnosed active respiratory tuberculosis disease does occur in health care settings.Īll health care settings should have a tuberculosis management or infection prevention and control program in place. The incidence of active tuberculosis in Canada is generally low. NAAT may also be performed in smear-negative patients.take at least 1 respiratory sample with Health Canada-approved or -validated in-house NAAT in all new, smear-positive cases.nucleic acid amplification testing (NAAT).rapid molecular tests for DST should be reserved for patients with a high pretest probability of multi-drug-resistant tuberculosis.phenotypic DST should be routinely performed for all first positive culture isolates obtained from each new tuberculosis case.culture results typically take 2 to 8 weeks.every specimen sent for smear microscopy should be set up for culture in 1 solid and 1 liquid medium.mycobacterial culture and phenotypic drug sensitivity testing (DST).same-day collection may be considered to reduce patient drop-out.sputum (phlegm) specimens should be collected a minimum of 1 hour apart.everyone with suspected tuberculosis should undergo testing with at least 3 concentrated fluorescent smears.it should be followed by microbiological tests for tuberculosis.chest radiography cannot provide a conclusive diagnosis on its own.In Canada, the standard testing algorithm for active tuberculosis includes the following tests: do a complete medical history and examinationĮvery effort should be made to obtain a microbiological diagnosis.There are 3 steps in diagnosing active tuberculosis disease: when an individual is considered to be at high risk.in everyone with signs and symptoms of tuberculosis.Testing for active tuberculosis is indicated: not recommended for routine diagnosis of latent tuberculosis infection.it takes 3 to 8 weeks after exposure for the skin test to become positiveīlood test (interferon gamma release assay)Ī blood test for latent tuberculosis infection is:.recently been infected by a person with active tuberculosis disease:.infected with other tuberculosis -like germsĪ negative test result can happen even if a patient has tuberculosis bacteria in their body.vaccinated with Bacille Calmette-Guérin vaccine (BCG).In the presence of symptoms or abnormal chest X-ray, sputum for acid-fast bacteria smear and culture should be taken.Ī positive test can happen even if a patient does not have a latent tuberculosis infection. assess signs and symptoms suggestive of possible active tuberculosis disease.do more tests to find out if the patient has active tuberculosis disease.investigate further to rule out a false positive.If a patient has a positive test result, you may need to: Inform your patient if the test is positive or negative. A measurement of more than 5 mm could be considered a positive result. The area of hardness (not redness) should be objectively measured with a ruler. The spot where the needle was injected will develop an area of redness with possible hardening (induration). 
If the patient is infected with tuberculosis, a skin reaction will occur within 48 to 72 hours.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
